Obesity and diabetes are two highly related conditions, meaning one can cause or be a result of the other. In addition, obesity and diabetes can both together and individually be precursors to other, more serious conditions like liver disease, cardiovascular issues, digestive problems, certain cancers, and more.
Dr. Bradley Freilich, the founder of Kansas City Research Institute (KCRI), is a widely published, board certified gastroenterologist and hepatologist. He is passionate about offering resources and positive guidance for liver disease patients through the power of research.
With the help of his dedicated team, Dr. Freilich works to bring safe, reliable, and groundbreaking treatment opportunities to fatty liver patients from all over the Kansas City metro. Often this starts with treating precursory conditions like obesity and diabetes.
Continue reading to learn more about how obesity and diabetes function, and liver treatment options available to you in Kansas City.
What is obesity?
Obesity refers to an excess of body fat but is usually much more complex. Medical obesity is often quite convoluted in its causes, contributors, and related complications. Being obese is a major comorbidity to many other health issues you may have, so it is important to recognize its impact on your overall health and know when to seek help.
Signs and symptoms
For many people, the earliest signs of obesity are cosmetic. Changes in your weight or body shape can often be determined without medical assistance.
Body Mass Index (BMI) is the most common tool for diagnosing obesity. Your BMI is a value derived from your height and mass used to place you in one of four categories: underweight, normal, overweight, or obese.
Causes of obesity
The most basic cause of obesity is calorie surplus, meaning you consume more calories than you burn in average daily activity. Your body stores these extra calories as fat, which builds over time.
It’s important to note that the causes of obesity can be complex and include genetic, environmental, behavioral, metabolic, and hormonal factors.
Specific risk factors may include, but are not limited to:
- Family inheritance and influences, genetic or behavioral
- Lifestyle choices like poor diet and inactivity
- Other health conditions and medications
- Social and economic issues
- Age
- Pregnancy
- Stress
- Lack of sleep
- Microbiomes, or gut bacteria imbalances
Diabesity: obesity as a precursor to diabetes
While diabesity is not a medical diagnosis, it is a term used to refer to the combined adverse effects of diabetes and obesity. Being obese causes insulin resistance over time, increasing your risk for developing diabetes ten-fold.
In a person with normal weight and insulin levels, the pancreas produces the proper amount of insulin necessary to transport glucose (blood sugar) through the blood. Insulin sends the glucose into your muscle cells, where it’s used to produce energy, or to your liver cells, where it’s stored for later.
When your cells are filled with excess fat, there is less room for incoming glucose, causing the cells to become glucose-resistant and excess glucose to remain in your bloodstream (high blood sugar). As a result, the pancreas overcompensates and produces even more insulin, which is not sustainable for the organ and causes damage and lowered insulin levels over time, leading to diabetes.

What is type II diabetes?
Glucose is the main sugar found in your blood. It comes from the food you eat and is an important ingredient in fueling your body. Your blood carries glucose to your cells, and insulin produced by your pancreas helps your cells use the glucose to create energy.
Type II diabetes is a chronic condition characterized by too much glucose circulating in the bloodstream and improper insulin production.
Signs and symptoms
Perhaps the most dangerous element of diseases related to the liver, namely type II diabetes, is that the onset of symptoms is gradual and often undetectable until significant damage has occurred. Individuals with type II diabetes may be living with their condition for years before they know it. This makes seeking diagnosis and treatment even more essential.
The most common symptoms related to type II diabetes include:
- Increased thirst
- Frequent urination
- Increased hunger
- Unintended weight gain/loss
- Fatigue
- Blurred vision
- Slow-healing sores
- Frequent infections
- Numbness or tingling in the hands or feet
- Areas of darkened skin, usually in the armpits and neck
Causes of diabetes
Type II diabetes results when two problems within the body occur together:
- Your pancreas is unable to produce enough insulin to manage your blood sugar level.
- Cells in your muscle, fat, and liver become resistant to insulin.
Researchers are unsure of exactly why or how these two problems occur, but there are a set of specific risk factors associated with type II diabetes.
Risk factors
These factors do not cause diabetes but may increase your risk of developing type II diabetes.
- Being overweight or obese.
- If you’re a man with a waist circumference above 40 inches or a woman with a measurement above 35 inches.
- Being less active. Physical activity helps control your weight, uses glucose as energy, and makes your cells more sensitive to insulin.
- If you have a direct family history.
- Although it’s unclear why, people of certain races and ethnicities—including Black, Hispanic, Native American and Asian people, and Pacific Islanders—are more likely to develop type II diabetes.
- High cholesterol is a prominent risk factor for diabetes and other cardiovascular conditions.
- Age, especially after 45.
- Prediabetes—a condition in which your blood sugar level is higher than normal, but not high enough to be classified as diabetes.
- There are pregnancy-related risks, like if you developed gestational diabetes when you were pregnant or if you gave birth to a baby weighing more than 9 pounds.
- Polycystic ovary syndrome—a common condition characterized by irregular menstrual periods, excess hair growth and obesity.
- Areas of darkened skin, usually in the armpits and neck, can indicate insulin resistance.
Complications related to diabetes
Potential complications, or comorbidities, related to type II diabetes include:
- Non-alcoholic Fatty Liver Disease (NAFLD)
- Heart and blood vessel disease
- Nerve damage
- Kidney disease
- Eye damage
- Skin conditions
- Slow healing
- Hearing impairment
- Sleep apnea
- Dementia
Ways to help prevent obesity and diabetes
There are plenty of healthy habits you can implement in your life to help prevent the onset of both obesity and diabetes.
- Eating a balanced diet. The number one healthy habit is to make sure your regular diet includes healthy food options like fruits, vegetables, and whole grains. Foods that are low in calories and high in fiber will keep your gut balanced.
- Regular exercise. Find an activity that suits you, like walking, biking, swimming, or jogging, and maintain at least a couple of hours per week of regular exercise.
- Maintaining a healthy weight. This is especially important for individuals who have been diagnosed as pre-diabetic. If you have questions, speak to your doctor about what a healthy weight looks like for your age and body type.
- Avoiding long stretches of inactivity. After a long period of inactivity, like sitting at a desk or watching a movie, getting up and walking around for a bit is an easy way to reduce your risk. Try to stretch your legs and get your blood flowing at least every hour, if not every 30 minutes.

How are obesity and diabetes linked to fatty liver disease?
Obesity and diabetes are both risk factors, and often precursors, for fatty liver disease (FLD)—a much more serious and much less treatable liver condition. FLD refers to complications that arise from an excess of fat stored in the liver. According to data from the Mayo Clinic, nonalcoholic fatty liver disease (NAFLD) affects about one quarter of the population in the U.S.
There are no FDA approved treatments for FLD, and it can progress quickly into more serious issues like end stage liver disease or cirrhosis in 25% of patients, even though it presents with no symptoms at all.
FLD is measured by degree or amount of scarring on the liver, also known as fibrosis. Obesity, insulin resistance, and diabetes may all be contributing factors to the formation of fibrosis, and therefore the progression of FLD. The effects of FLD cannot be reversed, but there are things you can do to prevent your fibrosis from progressing.
Look to KCRI for FLD treatment options
If your obesity and diabetes have progressed, or if you are concerned about their impact on your liver health, you can turn to KCRI for expert diagnosis technology and leading care options.
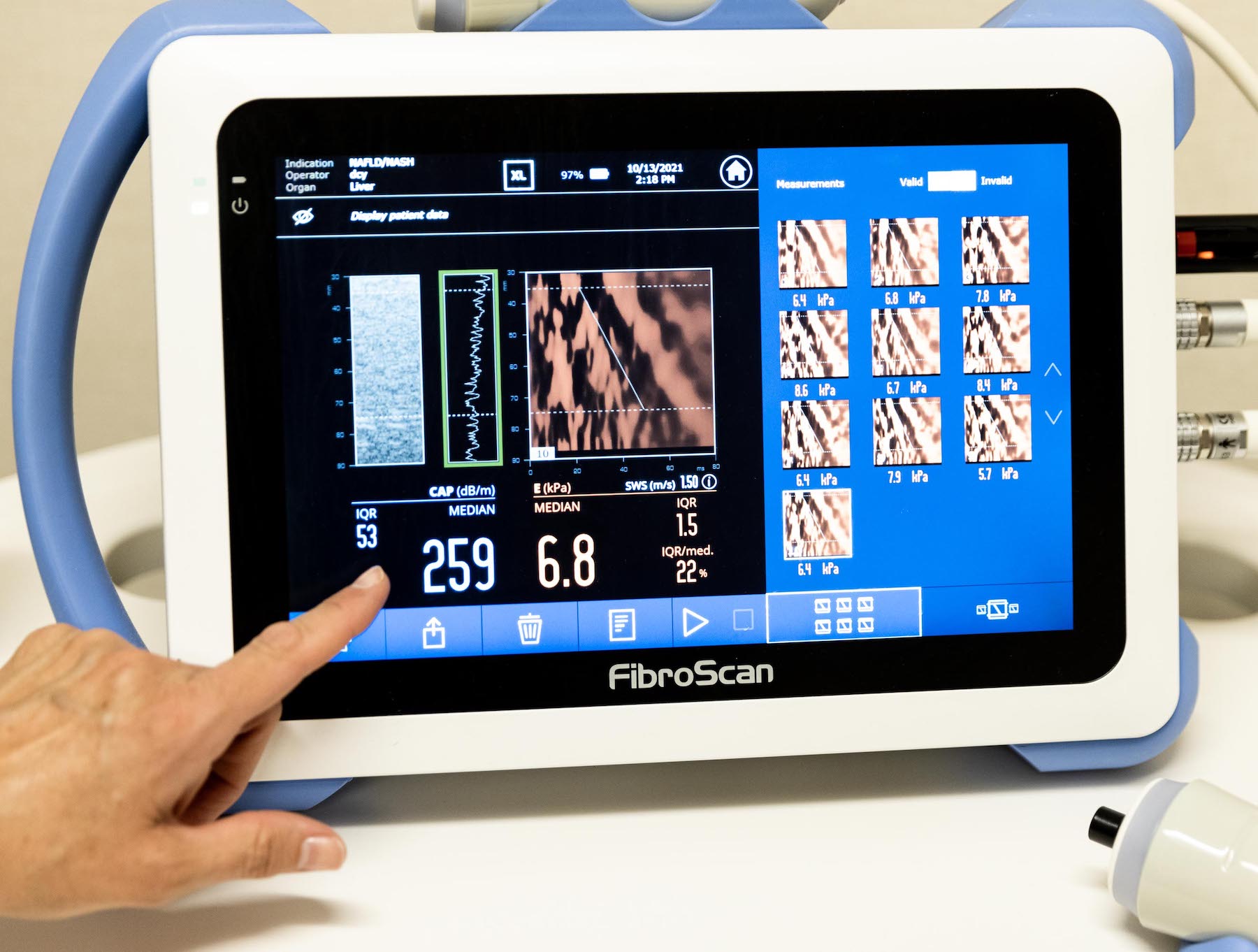
FibroScan
FibroScan is a non-invasive, gold-standard care solution for the comprehensive management of liver health. It is an alternative to liver biopsy, which is a more invasive procedure that uses a needle to retrieve a liver tissue sample. Because of this, using FibroScan can greatly improve treatment and care for patients who need continual reassessment of their liver condition.
FibroScan readings are useful in every step of identifying, treating, and reevaluating liver disease patients. FibroScan results are used to:
- Estimate the severity of existing liver damage (scarring, or fibrosis)
- Determine the amount of fat in the liver
- Guide prognosis and treatment
- Monitor liver disease progression and regression over time
Learn more about FibroScan near you →
Clinical trials
KCRI is the premier provider of fatty liver clinical trials in the Kansas City area. With us, you know that you are receiving the safest and most effective experimental drugs and procedures available. Just like we screen patients for candidacy, we screen trials for reliability and effectiveness. We only participate in trials with proven safety, minimal side effects, and proven success.
Because there are no FDA-approved treatments for FLD, and no cure for diabetes, a clinical trial is often a patient’s best or only option for effective disease relief.
If you are looking to join a clinical trial, there are multiple ways to begin your journey.
- Use the current research page on our website to stay informed about trials we are currently enrolling for
- Use our online Am I A Candidate tool or request a call to speak to one of our researchers
- Get a referral from a primary care physician based on your medical history

Metabolic weight loss program
Clinical trials may not be an option for everyone, but there are other treatment avenues for patients struggling with obesity and related conditions like hypertension (high blood pressure) and diabetes. Dr. Freilich also partners with HCA Midwest Health and Kansas City Gastroenterology & Hepatology Physicians Group (KCGI) to provide a metabolic weight loss program geared toward obese and at-risk patients.
Transforme Metabolic and Weight Management is a multi-disciplinary program designed to help patients achieve long-term weight loss goals and reduce their risk of chronic conditions linked to obesity. Because obesity is a common comorbidity for liver-related diseases for which there are no cures, Dr. Freilich and KCGI are committed to providing patients with additional support on their journey to better health.
Contact KCRI now for obesity and diabetes resources near you
Professionals at KCRI are dedicated to helping our patients manage and improve their symptoms with leading research and technology. If you are ready to learn more about obesity and diabetes resources near you, contact Kansas City Research Institute today to speak to a medical professional.
You can also use our Am I A Candidate tool to learn more about how your stage and symptoms might align with our available technology and treatments or schedule an appointment today.