What is Pancreatitis?
The role of the pancreas is to produce enzymes and hormones that aid in digestion and regulate the way your body processes sugar. Pancreatitis occurs when digestive enzymes become activated while still in the pancreas, causing inflammation. Pancreatitis can either be chronic or acute. Acute pancreatitis appears suddenly and lasts for a few days, while chronic pancreatitis develops over years causing life threatening complications.
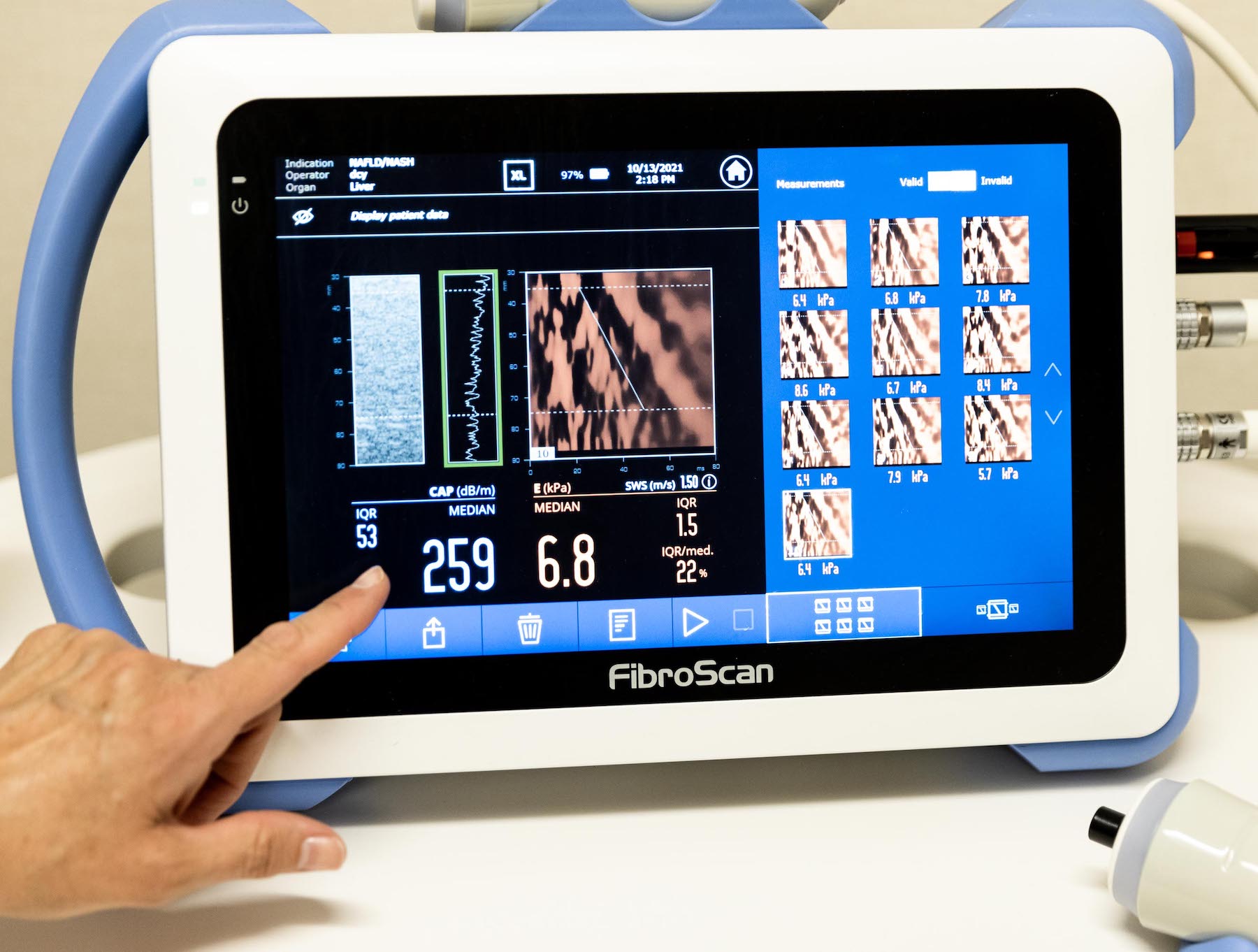
There are many factors that can cause pancreatitis including: gallstones, alcoholism, certain medications, obesity, abdominal surgery, infection, and pancreatic cancer. Blood tests, and imaging are tools that are used to help diagnosis and monitor progression. There is no cure for pancreatitis, however clinical trials may be an option for you to help manage your symptoms.
Risk Factors
- Diabetes
- Alcoholism (most common)
- Certain Medications
- Gallstones
- High Triglyceride Levels
- Family history
- Obesity
- Pancreatic Cancer
- Trauma
Symptoms
- Abdominal Pain
- Fever
- Rapid Pulse
- Nausea
- Vomiting
- Tenderness
- Weight Loss
- Oily, Smelly Stools (steatorrhea)
Treatments
- Pain Medication
- Intravenous (IV) fluids
- Endoscopic Procedure to remove obstructions in bile duct
- Endoscopic Procedure to remove damaged tissue
- Maintain a healthy diet
- Stop drinking alcohol
- Quit smoking
- Clinical trials

Managing Pancreatitis
Abdominal pain is often the first symptom of pancreatitis. This pain often causes patients to seek help from various medical providers. Your providers will run a series of laboratory tests, imaging, and often times you will undergo endoscopic procedures to determine the severity of the disease and develop a plan for your over treatment. Pain medication IV fluids are often the first course of action as they help address some of the symptoms of pancreatitis.
Once you are feeling better and are hydrated, your health care provider will discuss a treatment plan with you. Lifestyle modifications are often the first steps to take in your recovery. You can be proactive with your health by making the below lifestyle changes to help prevent symptoms and improve overall quality of life:
- – Stop smoking
- – Decrease alcohol consumption
- – Drink plenty of water
- – Eat a balanced diet that is low in fat
- – Try alternative pain therapies such as: meditation, exercise, yoga, acupuncture

Currently Enrolling
Trials at KCRI
FAQs about Pancreatitis
Frequently Asked Questions
How does KCRI diagnose pancreatitis?
KCRI does not diagnose pancreatitis. Typically, pancreatitis is first discovered when routine lab work reveals elevated levels of lipase, the pancreatic enzyme, or when patients experience abdominal pain that leads them to seek medical help.
What treatments are available for pancreatitis?
There are a few different solutions for both chronic and acute pancreatitis. Your provider may suggest or prescribe:
Fasting under medical supervision. This is one of the easiest and most common ways to alleviate inflammation of the pancreas.
- – Pain medication, which could be appropriate depending on your symptoms and health history.
- – Pancreatic enzymes, which aid in digestion.
- – Long-term pain management through nerve blockers.
- – Surgical procedures if necessary.
- – & more
KCRI also facilitates clinical trials for pancreatitis to help patients who are looking for new or alternative treatments. To find out if you are a candidate for any upcoming clinical trials, you can submit your information directly via our website.
Those that Participate:
- See a board-certified physician at no cost
- Have access to possible new treatment options before the general public
- May be compensated for time and travel