Your liver is your body’s largest internal organ, responsible for balancing and creating fuel for all of your other internal systems. As blood passes through, the liver breaks down and metabolizes essential nutrients, making them easier to use for the rest of your body.
Cirrhosis is the final stage of chronic liver disease where these necessary functions are interrupted by extensive tissue damage. For many patients, this is a daunting diagnosis.
Kansas City Research Institute (KCRI) is committed to bringing cirrhosis patients in Kansas City safe, reliable, and impactful treatment options to improve overall health and wellness. Keep reading to learn more about cirrhosis treatment and care.
What is cirrhosis?
Identified as the final stage of fibrosis (scarring) of the liver, cirrhosis is the final step before liver failure. As fibrosis progresses, scar tissue replaces healthy, active tissue in the liver, disrupting liver function. What characterizes specific liver conditions, including cirrhosis, is the degree and quality of this disruption to function.
Symptoms
Signs and symptoms of cirrhosis include:
- Tendency to bleed or bruise early
- Fatigue
- Jaundice or yellowing of the skin and eyes
- Ascites or fluid buildup in the abdomen
- Weight loss
- Itchy skin
- Edema or swelling
- Nausea
- Swelling in the legs
- Disorientation and drowsiness
- Slurred speech
- The development of spider-like vessels underneath the skin surface
- Gastrointestinal bleeding
It is important to note that because cirrhosis is the final stage of liver disease, symptoms of any precursory conditions could also be included as symptoms of cirrhosis. We always recommend consulting a medical professional about symptoms you are experiencing. Request a call if you would like to speak to someone from our clinic.

Starting points
The formation of fibrosis usually begins with a precursory condition before it progresses to cirrhosis. While these precursory conditions are often more treatable, it is important to seek medical guidance and be proactive about your diagnosis and treatment.
Alcoholism
Part of the liver’s job is to break down alcohol when you consume it. Drinking excessively causes the liver to take in more alcohol than it can process, causing damage to the tissue over time. As scar tissue continues to replace healthy tissue, the function of the liver reduces drastically, leading to cirrhosis.
Fatty liver disease
Fatty liver disease (FLD) refers to complications that arise from an excess of fat stored in the liver. FLD can progress quickly into more serious issues like end stage liver disease or cirrhosis in 25% of patients if left untreated, even though it presents with no symptoms at all.
Potential causes of FLD include obesity and diabetes, high cholesterol, metabolic syndrome, diet, and other genetic factors.
Non-alcoholic fatty liver disease
Non-alcoholic fatty liver disease (NAFLD) often presents the same way as FLD but excludes patients who report alcohol consumption. NAFLD affects about 25% of the population in the U.S. and can also progress into cirrhosis if left untreated. Clinical trials are often NAFLD patients’ best and only option for treatment.
Non-Alcoholic Steatohepatitis
Non-alcoholic steatohepatitis (NASH) refers to inflammation of the liver caused by excess fat. As it progresses, this inflammation can lead to scarring and damage to the liver over time. NASH can also be caused by obesity, metabolic syndrome, and high cholesterol.
Primary Biliary Cholangitis
Primary Biliary Cholangitis (PBC) is more commonly referred to as chronic liver disease. PBC falls under the autoimmune category and directly affects the bile ducts of the liver, causing inflammation that can lead to fibrosis.
Autoimmune Hepatitis
Autoimmune hepatitis is a condition where your body’s natural immune system, typically responsible for fighting off disease, attacks your liver cells instead. The condition can become chronic and cause long-term damage. It is unclear what causes autoimmune hepatitis, but it is most often diagnosed in individuals with other autoimmune disorders.
Viral Hepatitis
Viral hepatitis is liver damage and inflammation caused by a viral infection. The most common viruses linked to viral hepatitis are hepatitis A, B, C, D, and E. These viruses can be spread through contaminated food and drink or exposure to contaminated bodily fluids like blood and stool.
Alpha-1 Antitrypsin Deficiency
Alpha-1 antitrypsin deficiency is a genetic condition that increases your risk for both liver and lung disease. Your liver is responsible for producing the protein alpha-1 antitrypsin (AAT) and sending it to the lungs. If the proteins produced are the wrong shape, they get stuck in the liver and are not able to make it to the lungs where they protect against disease and damage.
Hemochromatosis
Hemochromatosis is a condition that causes your body to absorb an excess amount of iron from the food you eat. The excess iron is stored in your organs, especially the liver, heart, and pancreas and causes damage as it builds up.
Staging
Cirrhosis is further classified based on its severity. More generally, it is either compensated or decompensated and these stages are progressive.
Compensated cirrhosis is often asymptomatic. Patients will not exhibit typical indicators like ascites, variceal hemorrhage, hepatic encephalopathy, or jaundice. The key prognostic factor for compensated cirrhosis patients is the presence of varices—abnormally enlarged veins in the esophagus that are caused by blood clots or blockages in the liver.
We identify decompensated cirrhosis by the overt presence of symptoms or complications. With effective cirrhosis treatment and disease management at KCRI, decompensated patients may be able to regress to the asymptomatic stage.
Scanning
When dealing with cirrhosis treatment, the primary method of liver assessment is scanning. There are multiple types of scans used to target the liver, including FibroScan, a painless alternative to liver biopsy.
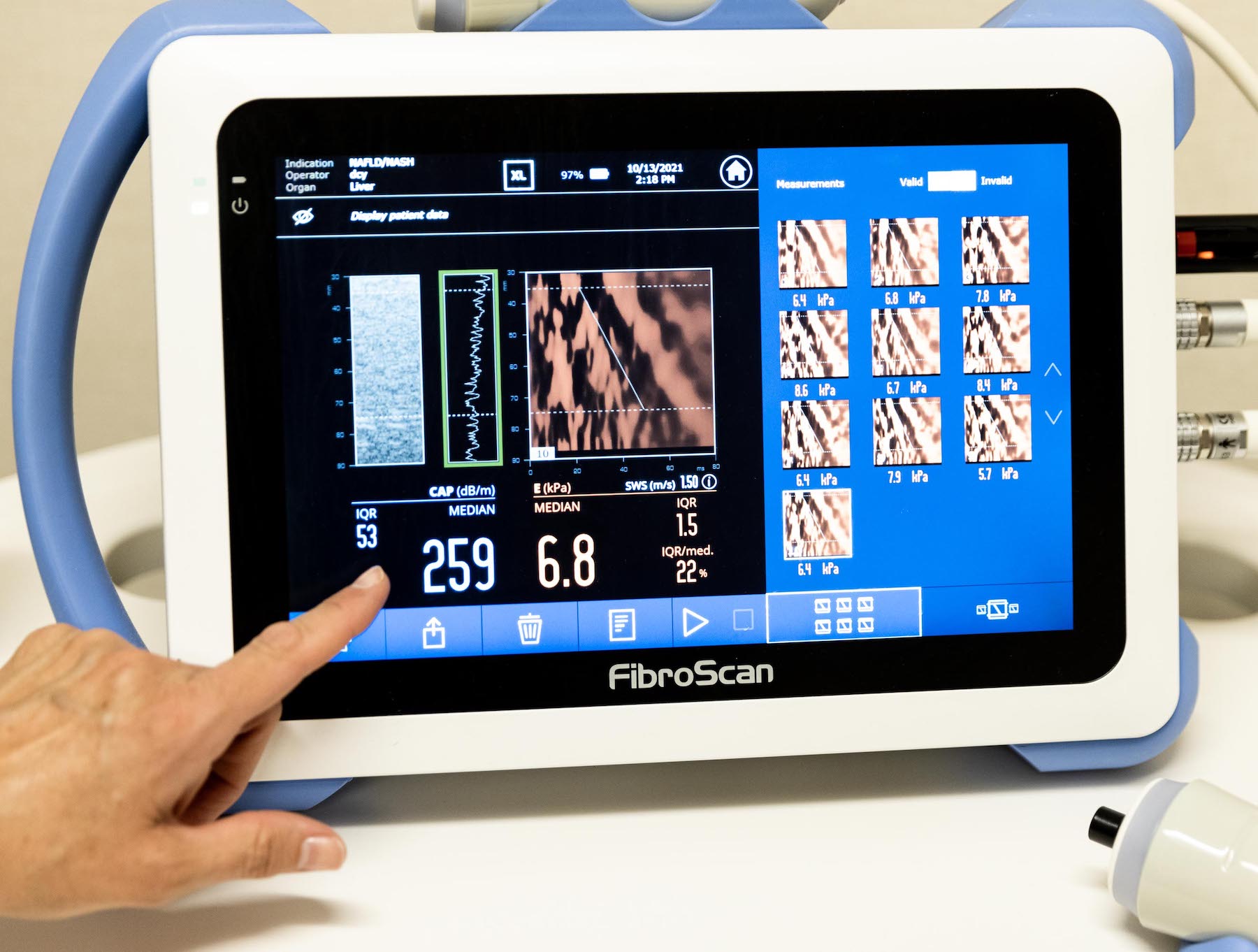
About FibroScan
FibroScan is a non-invasive device used to assess liver health. It measures the degree of fibrosis, or scarring, on the liver that could be caused by a number of liver conditions.
The device measures fibrosis based on the “hardness,” or stiffness, of the liver using a probe similar to an ultrasound. This measurement is given in kPa, which is a unit of pressure. Once we determine the degree of fibrosis, we can recommend further testing, treatment options, clinical trials, and more.
FibroScan technology is fast and intuitive. The exam can be performed in-office by any medical professional in under 10 minutes, providing immediate results at the point of care.
We use FibroScan to reach a diagnosis or measure the status of a multitude of conditions affecting the liver, including:
- Chronic Hepatitis B
- Chronic Hepatitis C
- Fatty Liver Disease (FLD)
- Non-alcoholic Fatty Liver Disease (NAFLD)
- Cirrhosis
- Liver failure
- Metabolic syndrome
- Autoimmune diseases
Learn more about FibroScan near you in Kansas City →
Other types of scans and testing for liver disease and cirrhosis treatment include:
- Computerized Tomography (CT) Scan
- Magnetic Resonance Elastography (MRE)
- Magnetic Resonance Imaging (MRI)
- Blood testing
- Liver biopsy
Is cirrhosis preventable?
On some levels, yes. It is impossible to protect yourself from genetic conditions, like cystic fibrosis or hemochromatosis, that may contribute to liver disease; however, employing basic healthy habits is an easy way to prevent or slow the development of fibrosis.
Keeping an active lifestyle and healthy diet, including limiting your alcohol consumption, are natural ways that you can evade the development of precursory conditions to cirrhosis like FLD and NAFLD.
Abstaining from illicit drugs and practicing safe sex are additional healthy habits to avoid contracting harmful diseases, like hepatitis and autoimmune deficiencies that can harm your liver.
In addition to clinical trials, KCRI offers lifestyle modification programs and advice to help patients manage cirrhosis symptoms and limit any further damage to their liver.
Cirrhosis treatment options
While cirrhosis cannot be reversed, the goal of cirrhosis treatment is to slow the progression of scarring and manage symptoms. Depending on the stage of your condition, treatment may be focused on underlying causes, like alcohol dependency or precursory conditions, or resulting complications, like portal hypertension or encephalopathy.
Liver transplant surgery
If your cirrhosis is extremely advanced, where liver function is bordering on failure, you may become a candidate for a liver transplant surgery. This procedure involves either replacing your diseased liver with a healthy organ from a deceased donor or replacing a portion of your liver with a healthy portion from a live donor.
Candidates for transplant must go through extensive testing to determine if they are healthy enough to have a successful outcome. In most cases, patients with liver failure as a result of alcohol use are not candidates for transplant surgery.
Clinical trials
Because there is no cure for advanced cirrhosis, clinical trials are often a patient’s best and only option to receive impactful treatment for their disease.
If you are seeking cirrhosis treatment and aren’t sure where to turn, KCRI can guide you through the process of applying for a clinical trial and help you access leading medical research.
If you are looking to join a cirrhosis clinical trial, there are multiple ways to begin your journey.
- – Use the current research page on our website to stay informed about trials we are currently enrolling for.
- – Use our virtual Am I a Candidate tool get pre-screened or request a call to speak to one of our researchers.
- – Get a referral from a primary care physician based on your medical history.
The difference in phase II and III clinical trials
KCRI patients can rest easy knowing that our medical staff is committed to advancing medicine by facilitating access to promising new treatments.
- Phase I – Screening for the safety of the drug or therapy in a small number of people
- Phase II – Testing the efficacy and safety of the drug or therapy in a larger number of people
- Phase III – Confirming effectiveness, monitor side effects, compare to commonly used treatments, and collect information that will allow the experimental drug or treatment to be used safely on large groups of people. Typically, 1000+ individuals are enrolled in Phase III studies.
All of our cirrhosis studies are in Phase II or III of clinical trials, meaning the protocol has already been through at least preliminary testing. The more advanced the phase of a clinical trial, the more reassurance we have in its effectiveness, and the easier it is for us to determine who would be an ideal candidate.
Learn more about our clinical trial process at KCRI →
Dr. Freilich and the KCRI difference
Dr. Bradley Freilich, the founder of KCRI, is a widely published, board certified gastroenterologist and hepatologist specializing in fatty liver disease and treatments. He is passionate about offering resources and positive guidance for liver disease and cirrhosis patients through the power of research.
With the help of his dedicated team, Dr. Freilich works to bring safe, reliable, and groundbreaking outpatient treatment opportunities to liver disease patients from all over the Kansas City metro. That’s our specialty, that’s our mission.
Contact KCRI now for cirrhosis treatment in Kansas City
Professionals at KCRI are dedicated to helping our patients manage and improve their symptoms with leading research and technology.
If you are ready to learn more about how cirrhosis treatment near you can impact your health and wellness, contact Kansas City Research Institute today to speak to a medical professional, or use our virtual candidacy tool to get pre-screened for our clinical research.